by John McGrath
Ashley Holman, MD, Innovation in Education begins with a simple but powerful question: How do you prepare physicians to do something well before doing so under the pressure of clinical practice?
As an associate professor of anesthesiology at Michigan Medicine, Holman spent years advancing the use of awake spinal anesthesia for infants and young children.
This technique may reduce perioperative risk, shorten recovery time, and improve outcomes for some younger surgical patients.
But as he helped establish this clinical practice, he began to see another challenge emerge—although the technique was effective, the opportunity to learn it was limited.
“Ac pediatric spinal anesthesia is not something that most residents encounter during standard training,” Holman said.
“At some institutions, even pediatric anesthesia fellows can graduate without having seen one performed, let alone gained enough experience to feel comfortable enough to perform the procedure themselves independently.”
This gap in training has become the catalyst for a new kind of innovation, one centered not on the operating room, but on how physicians learn before stepping into it.
Using an innovation research grant from the University of Michigan Medical School’s Office of Graduate Medical Education, Holman designed a structured training pathway that combines formal instruction with hands-on simulations and progressive clinical exposure.
The program focuses on teaching the entire pediatric spinal anesthesia process, from patient positioning and anatomical recognition to needle handling, drug delivery, and team-based stabilization techniques that are rarely included in standard residency training.
Building confidence before the first case
The training program is designed to introduce pediatric spinal anesthesia through a deliberate, step-by-step learning process.
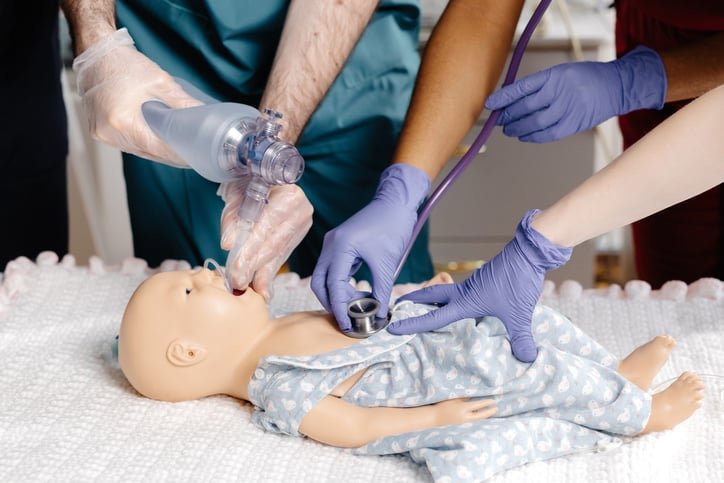
Rather than relying on first attempts at pediatric spinal anesthesia in a stressful operating room, trainees begin by learning positions, anatomy, and techniques in a quiet simulation environment, where they can repeatedly practice, receive feedback, and refine their approach before transitioning to the supervised clinical field.
“In adult anesthesia, you can talk a patient through what you’re doing. You can tell them to be still. With children, that’s not an option,” Holman said.
“They’re moving, they’re crying, and the margin for error is much smaller. The simulation gives students a chance to build muscle memory and confidence before performing the procedure on a real patient.”
Bringing training to national level
What began as a local educational effort has grown into a model both institutionally and internationally.
Within Michigan Medicine, pediatric spinal anesthesia has expanded from a single urologist to include multiple surgeons in urology, as well as pediatric surgery, plastic surgery and orthopedic surgery.
The program has also been expanded to Sparrow Hospital in Lansing, so that children there can benefit from the technique.
“One of the most rewarding parts of this journey is seeing people take it to their own organizations and create something new,” Holman said.
“I’ve mentored faculty to start spine programs at St. Vincent in Toledo, Henry Ford Hospital and Corwell Health in metro Detroit, the University of Utah, Pennsylvania State University, Medical University of South Carolina, AIC Kizabe Hospital in Kenya, and other institutions. Seeing them adapt to the patients and the way the patients are worked is more impactful than we could do on our own.”
That changes learned habits
This confidence, built through structured training and deliberate practice, is an important part of patient safety.
“When clinicians feel prepared, they are more focused, more specific and better able to respond to what’s happening in front of them,” Holman said. “It’s good for students, and it’s even better for patients.”
“At its core, this work is about access to knowledge, training and ultimately safe care,” Holman said.
“If we can help more physicians feel confident and prepared, then we’re doing something meaningful.”
Learn more about Innovation in medical education at the University of Michigan.
–
Previously published Also at michiganmedicine.org Creative Commons License
***
–
The world is changing fast. We help keep you.
We will send you 1 post, 3 times per week
All premium members can watch The Good Men Project without any ads. Need more information? A full list of benefits is here.
–
Photo credit: iStock